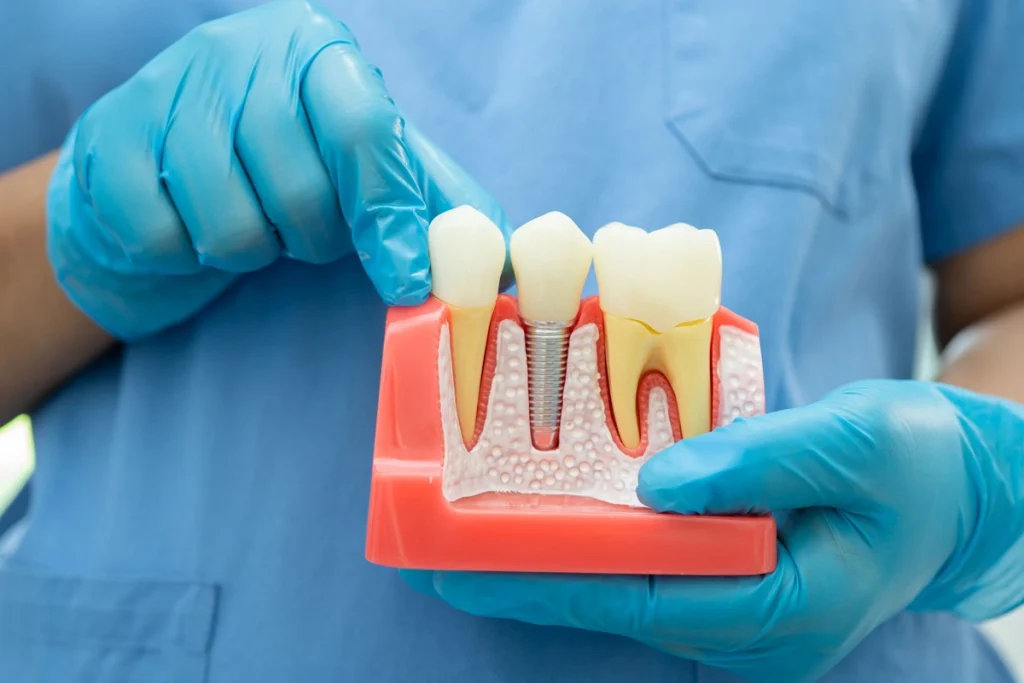
Dental implants replace missing teeth using prosthetic systems. Patients lose teeth due to decay or injury, and clinicians evaluate implant options based on oral conditions. When teeth are missing, jawbone structure may change, and dentists assess whether implant placement is appropriate. Dentists evaluate bone structure before treatment, and they determine implant suitability based on clinical findings. When diagnostic evaluation is complete, clinicians select implant types according to anatomical conditions, and treatment planning follows established implant classifications.
Placing Dental Implants
Endosteal dental implants place titanium posts directly into the jawbone. Dentists use this method when bone volume supports placement, and the implant integrates with surrounding bone during healing. After placement occurs, a crown attaches to the implant, and this restores chewing and speech function. When sufficient bone exists, clinicians proceed with implant placement, and they evaluate healing before final restoration. If bone volume is limited, providers may recommend grafting procedures, and they assess whether the site can support long-term placement. Because implant integration depends on contact with bone, clinicians monitor stability during the healing phase, and they confirm readiness before completing restoration.
Bone integration requires a healing period. Clinicians evaluate bone response during this phase, and they track implant stability over time. When integration is complete, providers attach the final crown, and they restore function to the missing tooth area. Because dental implants depend on bone fusion for support, clinicians confirm structural readiness before final prosthetic placement.
Placing Subperiosteal Implants
Subperiosteal dental implants sit above the jawbone under gum tissue. A metal framework rests on the bone surface, and posts extend through the gums to support prosthetic teeth. This method supports patients with reduced bone height, and it avoids direct placement into the jawbone. When bone height is insufficient for standard implants, providers select this approach, and they use imaging to evaluate jaw structure. The framework is custom-fitted to the patient’s anatomy, and it is positioned over the bone to support prosthetic attachment. Because placement does not rely on deep bone integration, clinicians use this method when traditional implant placement is not possible, and they verify fit before proceeding with restoration.
Placing Zygomatic Implants
Zygomatic dental implants anchor into the cheekbone instead of the upper jaw. Surgeons place longer posts into the zygomatic bone, and this provides support when upper jaw bone cannot hold standard implants. This method is used in cases of severe upper jaw bone loss, and it allows implant placement when other options are not viable. When traditional upper jaw placement is not possible, clinicians evaluate the zygomatic bone, and they determine implant positioning using imaging. Because the cheekbone provides dense structural support, it allows implant stability during function, and it supports prosthetic attachment in cases of advanced bone loss.
Visit a Clinic
Dental implant systems restore oral function after tooth loss. Endosteal, subperiosteal, and zygomatic implants address different structural conditions, and clinicians select options based on patient anatomy. Implant selection depends on bone availability, and providers evaluate each case using diagnostic imaging and assessment. When patients receive implants, dentists match implant type to structural conditions, and they base decisions on evaluation findings. Because each implant category addresses specific anatomical needs, clinicians follow established treatment classifications, and restoration planning follows clinically defined implant selection criteria. Visit a clinic in your area to get started.